


Published on Apr 08, 2022
Multiplan (MPLN) says that it provides “independent, fair, and reasonable” pricing for out-of-network healthcare services. Previous Capitol Forum reporting showed that Multiplan’s pricing is not independent, as it can be manipulated by insurers. According to Capitol Forum’s ongoing investigation, Multiplan’s pricing is also not “fair and reasonable,” as the pricing appears to be based on […]
Multiplan (MPLN) says that it provides “independent, fair, and reasonable” pricing for out-of-network healthcare services.
Previous Capitol Forum reporting showed that Multiplan’s pricing is not independent, as it can be manipulated by insurers.
According to Capitol Forum’s ongoing investigation, Multiplan’s pricing is also not “fair and reasonable,” as the pricing appears to be based on maximizing profits, and, in one case, Multiplan admitted that, when setting prices, it relied on how much Multiplan discounted from the provider’s previous billed charges. Basing pricing on the percentage discounted from a provider’s previous charges is not a process that could reasonably be described as yielding “independent, fair, and reasonable” pricing for healthcare services, but it is perfectly logical for Multiplan since the company is paid based on the percentage difference between billed rates and prices paid by insurers.
Multiplan argues that its services that bring in “shared savings” fees help employers and patients, but when Multiplan cuts the rates for healthcare claims, either the employer is hurt by an increase in fees or the patient is hurt by receiving a large “balance bill.”
For this article, we focus primarily on three medical billers’ interactions with Multiplan.
One biller showed how Multiplan punished him for lowering his billing rate and rewarded him for raising his billing rate.
Another biller showed how Multiplan pricing left patients with big increases in out-of-pocket costs for physical therapy services.
Another biller described the process of Multiplan’s pricing as difficult to manage, opaque, and dramatically lower than pricing done by non-Multiplan-affiliated plans.
Each of the billers emphasized the amount of administrative time and expense that was necessary to deal with Multiplan-facilitated claims and to educate patients about unexpected increases in their portion of the bill.
For this part of its investigation, The Capitol Forum reviewed redacted “fee negotiation” communications between Multiplan and providers, insurance claim payment remittances, and documents filed in several lawsuits, including depositions, trial transcripts, and exhibits; interviewed several providers and owners of medical billing companies who spoke under the condition of anonymity because of concerns about retaliation from Multiplan and payors; read online provider complaints posted by providers; and interviewed a former Multiplan fee negotiator.
Multiplan spokesperson’s comments. “All of our pricing methodologies are fair, transparent and reasonable. Multiplan absolutely does not encourage providers to overcharge for their services—that is completely in opposition to our mission and would not be tolerated by us or by our clients,” a Multiplan spokesperson told The Capitol Forum in an emailed statement.
The Multiplan Billing Experience vs. the Typical Health Plan Billing Experience
Whereas a typical health plan sets an allowable rate for a healthcare service, some health plans first route out-of-network claims to Multiplan’s “negotiating services.” In effect, a provider sends a bill to the insurance plan, the plan routes the claim to Multiplan who offers an “adjusted price” (or “negotiated rate”) as part of a negotiation. Providers told The Capitol Forum that the adjusted price offer is a take-it-or-leave-it proposal. If the provider accepts the adjusted price, then the provider agrees not to balance bill.
This creates an unusual circumstance when there is a large gap between the billed charge and agreed negotiated rate. When setting future adjusted prices for a provider’s claims, Multiplan appears to rely on the percentage discounted from the billed charge rather than a specific dollar amount for a given service. When a provider decides to bill a subsequent claim for the same service at Multiplan’s previously accepted adjusted price, Multiplan responds with an almost proportionately lower adjusted price offer.
Effectively, negotiated rates with Multiplan, after the first negotiation, are phantom rates because Multiplan appears to stabilize the percentage gap between what a provider bills and the adjusted price the provider accepts. The provider knows what adjusted price Multiplan offered previously, but the provider will not be offered the same adjusted price again unless the billed charges remain at an inflated amount.
If the provider rejects Multiplan’s negotiated rate, the claim is paid much lower than the typical allowable rate which results in the provider balance billing the patient for the difference between the billed price and the allowable rate.
Here are some examples of out-of-network claims sent to health insurance plans that use Multiplan pricing services and the end results of those negotiations with Multiplan.
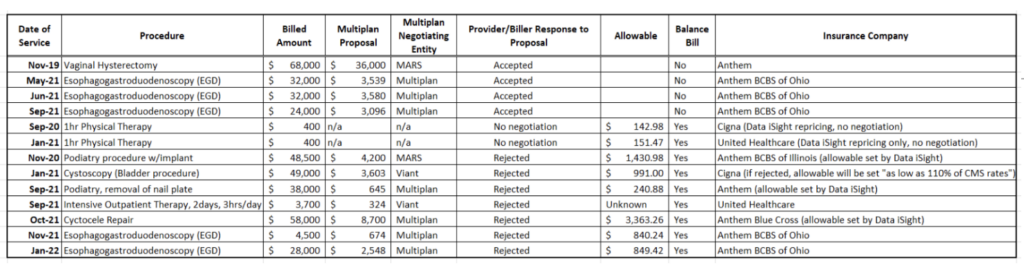
Source: Multiplan-facilitated negotiated or repriced out-of-network claims, according to interviews with billers and redacted documents reviewed by The Capitol Forum
Employers who self-fund health plans for employee health coverage pay insurance companies to administer the plan. The insurance companies charge employers fees, including fees for out-of-network claim management services and, when Multiplan is involved, the insurance company shares a portion of that fee revenue with Multiplan.
If the provider accepts Multiplan’s negotiated payments, then the employer pays high “shared savings” fees to the insurance company administering the health plan. Shared savings fees are based on a percentage of the amount between providers’ billed charges and the negotiated amount shown on the claim statement. Previously, The Capitol Forum reported on employers’ dissatisfaction with the shared savings fees.
Case Study 1: Biller for Surgery Centers
A biller who works in a western state with surgeons and surgery centers for specialties including neurosurgery, bariatrics, and gynecology, told The Capitol Forum in an interview, “The typical allowable rate received by our facility for complex upper endoscopy procedures performed prior to bariatric surgery was between $6,000 and $8,000. However, Multiplan and Anthem (ANTH) refused to honor that price unless we billed three to four times higher” than the negotiated rate.” So, the biller said he typical billed between $18,000 to $28,000—and sometimes as high as $32,000—to get paid between $6,000 to $8,000 from the Multiplan-affiliated health plans.
Then, in May 2020, the biller said Multiplan suddenly reduced its negotiated price to $3,539. The biller billed $32,000 to get the $3,539 adjusted price from Multiplan. He agreed to accept that rate as full payment and promised not to balance bill, as is required when providers accept a negotiated rate offered by Multiplan.
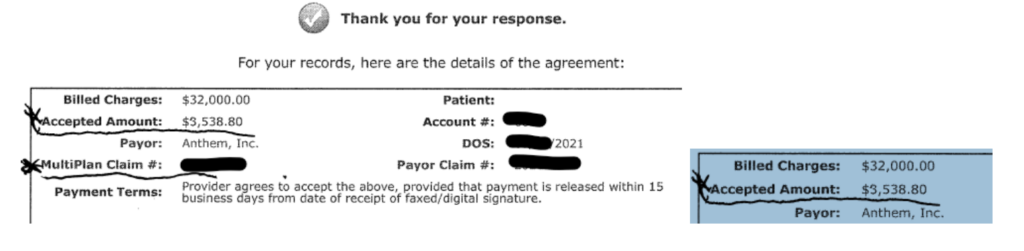
Source: Redacted Multiplan negotiation agreement
In June 2021, the biller dropped his price to $24,000, and Multiplan dropped its negotiated rate to $3,096, which the biller accepted.

Source: Redacted Multiplan negotiation agreement
Finally, in November 2021, the biller dropped his billed rate to $4,500 because he no longer wanted to choose between writing off larger amounts and balance billing patients. The biller anticipated that Multiplan’s negotiated rate of $3,096 or $3,539 would leave a more manageable $1,000 or $1,500 to write off or to balance bill to the patient.
But, instead of offering close to the previous adjusted prices of $3,096 or $3,539, Multiplan responded to the provider’s price cut by slashing the negotiated rate down to $673.65.
 Source: Redacted Multiplan negotiated offer
Source: Redacted Multiplan negotiated offer
In voicemails left by a Multiplan negotiator, the biller said he was told, “the claim is set at the same rate, as far as percentage goes. I am not able to increase it due to the maximum allowed amount.” According to the biller, the Multiplan negotiator in a follow up call “confirmed that the previous rate of $3,500 will not be offered until I increase the billed total.”
The biller persisted in asking questions about the formula Multiplan used to justify a decrease in the offered rate from $3,500 to $673.65 for the same procedure. He said the negotiator explained, “The allowable amount percentage is based on the percentage you had accepted in previous Anthem claims for similar plan and similar procedures.”
In reality, the new Multiplan payment was roughly 15% of the billed amount, whereas the previous offers were roughly 13% and 11% of billed charges, so it is unclear what the Multiplan representative meant by saying “the rate was the same, as a percentage.” But the explanation does indicate that, rather than independently assessing a “fair” price, Multiplan adjusts negotiated rates to maintain the percentage gap between billed charges and the offered price.
In a subsequent claim, the biller raised the charge to $28,000, and Multiplan increased the amount it offered to $2,548, thereby rewarding him for raising the price more than sixfold.
Anthem did not respond to a request for comment.
Physical Therapy
A medical biller for several physical therapists in the northeast told The Capitol Forum that they bill around $400 for an hour long out-of-network follow-up visit which, the biller said, is a rate many insurers accept. That means that a patient covered by a health plan with out-of-network benefits can meet a $1,200 deductible in three visits because, for each visit, the plan credits a $400 allowable rate towards the deductible. After the deductible is met, for a plan that has a 60/40 split between the health plan and patient, the plan will pay $240 of the bill leaving the patient to pay the remaining $160. So, a patient covered by a plan that has a $400 allowable would pay $2,320 for 10 follow-up physical therapy visits.
But for claims processed by Multiplan, the allowable rate is set at $151. The patient is still obligated to pay the provider $400 every visit but, since only $151 applies towards the deductible, it would take eight visits to meet a $1200 deductible. After the deductible is met, for a Multiplan-affiliated plan that is a 60/40 split between plan and patient, the plan only pays $91 for each visit, leaving patients to pay the remaining $309. So, 10 follow-up physical therapy visits would cost a patient covered by a plan that uses Multiplan close to $3,800.
That type of jump in out-of-pocket costs for patients can damage the relationship between the patient and healthcare provider and can cause patients to grow frustrated with their employer who provides the insurance.
The medical biller explained that she started seeing the drop in allowable for certain plans at the beginning of 2021. The allowable rate was reduced by Data iSight, Multiplan’s repricing service, and that she has not seen any negotiated offers. She said she has been making a lot of calls to Multiplan and Data iSight and Viant, which are companies under Multiplan’s umbrella, to ask questions and to help her patients get the benefit of the higher premiums they are paying for health plans with out-of-network benefits.
It is a challenge, she said, because the Multiplan representatives only allow her to ask five questions per call whether they can answer the questions or not.
Addiction Treatment Centers
An executive at a company that manages billing for addiction treatment centers located in multiple states told The Capitol Forum, “Multiplan is not the worst offender, Viant is much worse!” Although her company has dealt with Multiplan and Viant for years, she was unaware that Viant is a Multiplan company. Several sources who spoke to The Capitol Forum were under the impression that Viant, Medical Audit and Review (MARS), Data iSight, and Multiplan were unrelated companies.
The addiction treatment center biller said she “feels defenseless against [Multiplan and Viant].” She added that her peers in the addiction treatment industry feel the same way.
An example provided by the biller shows a negotiated offer from Viant on a claim for two days of intensive outpatient group therapy at three hours a day. The patient’s plan, which is managed by United Healthcare “states it pays 80% of usual and customary rates,” she said. “I averaged the out-of-network amount we see for the same service from UnitedHealth plans that have the same usual and customary rate language and don’t use Viant. The average comes to $924.”
The claim was billed at $3,700. Viant offered $323.58, according to the redacted negotiated offer reviewed by The Capitol Forum.

Source: Redacted Viant negotiated offer
Some insurers actually publish their allowable rates, she said. “We have asked on multiple occasions how [Multiplan and Viant] determine what gets sent out for pricing,” she said. “They will not divulge what their methodology is. Typically, we get a representative who says they have no control over what gets sent out for Multiplan pricing.”
“When we reject a negotiation, it takes months to get any payment and we never get paid more than the amount on the negotiation offer. Anytime we say no, we are stuck waiting for payment.” She added that sometimes she noticed “for the same patient and the same provider, one claim will be priced by Multiplan and a different claim is priced by the payor. We’ve called on these before and were informed that the higher priced claim was incorrect, and a recoupment will follow.”
The addiction treatment industry overall has actually been dealing with concerns about Multiplan for years. In a 2016 article in Sober World, an owner of California addiction treatment centers wrote, “As the major insurance companies don’t like paying for effective addiction treatment, they are using companies owned by Multiplan to reprice California’s small, non-medical treatment facilities using irrelevant data from Medicare.”
In recent years, addiction treatment providers have filed numerous lawsuits against Multiplan and insurers for underpaying claims. The cases are in active litigation.